Biological 3D printer achieves breakthrough in printing human body parts for surgical attachment
03/08/2016 / By Greg White
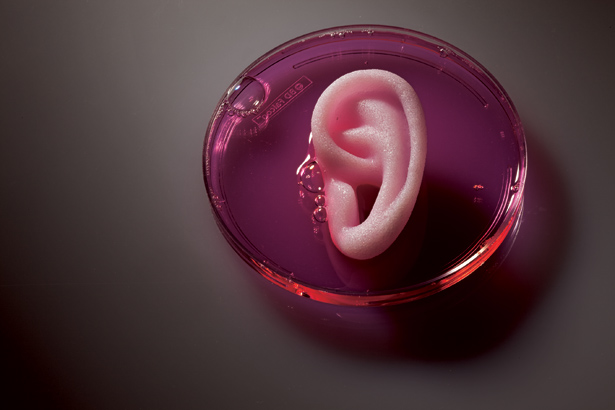
3D printed tissues and organs no longer exist solely in science fiction films like The Fifth Element. Scientists have created the first 3D printed ear, which puts literal blood on the tracks for the future of printed body parts.
The researchers were able to accomplished this with a newly developed 3D printer, which replicates the muscle structures that blossom into tissue after being inserted into animals.
Scientists have been looking into bio-printing as a way to restore damaged tissue for years. Duplicating the intricacies of human flesh is by no means easy. Nevertheless, with the use of bio-inks and multiple purpose built prints, engineered human tissue is now possible.
Researchers at Wake Forest Baptist Medical Center used this technology to create implants that matched the strength and size of human issue. It has taken researchers more than a decade to accomplished this goal.
Surpassing the limits of conventional bio-printing
The group’s Integrated Tissue and Organ Printing System (ITOP) is said to conquer the challenges of other bio-printing methods. It uses water-based gels that harbor cells and other biodegradable polymers, which are arranged in a specific pattern and a short-term outer structure.
The water-based gels were utilized to aid cell growth and health. In addition, the micro-channels provided nutrients and oxygen from the body to the system, which enabled it to stay alive while its blood system matured.
Researchers said that past engineered tissue structures devoid of blood cells needed to be tinier than 200 microns to help the cell survive. The new approach circumnavigates around this hurdle. The team used ITOP to create tiny ear structures 1.5 inches in length. They then inserted the implant under the skin of mice in a lab, which exhibited signs of vascularization in one to two months.
Testing the new tissue
To show that the engineered tissue mirrored a soft tissue structure, the researchers optimized the instrument to create muscle tissue and inserted it into rats. Within two weeks, it was strong enough to vascularize and trigger nerve formation.
In addition, the system printed a jaw bone fragment, which was large enough to be used for reconstructive surgery. In five months, the structures had developed into matured vascularized bone tissue.
“Our results indicate that the bio-ink combination we used, combined with the micro-channels, provides the right environment to keep the cells alive and to support cell and tissue growth,” Anthony Atala, senior author of the study, told sources.
The ITOP can also take information from CT and MRI scans, and create new tissue for patients. If a patient needs a particular kind of tissue for something like the segment of an ear or nose, the system could create an exact replica.
“This novel tissue and organ printer is an important advance in our quest to make replacement tissue for patients,” says Atala. “It can fabricate stable, human-scale tissue of any shape. With further development, this technology could potentially be used to print living tissue and organ structures for surgical implantation.”
More research needs to be conducted that examines the long-term results of this technology. The study was published in the journal Nature Biotechnology and was funded by Armed Forces Institute of Regenerative Medicine.
Sources include:
(1) DailyMail.CO.UK
(2) GizMag.com
(3) Nature.com
Tagged Under: 3D printing, ear transplant, genetically engineered tissue, Organ Printing System


















